Author:
Dr. Medvop Medical Team
Published Date:
26 Mar, 2026
Gingivoplasty
This article explains the medical purpose, evaluation process, procedural steps, risks, and recovery expectations associated with gingivoplasty, helping patients make informed decisions and understand when gum contouring may be recommended by dental professionals.
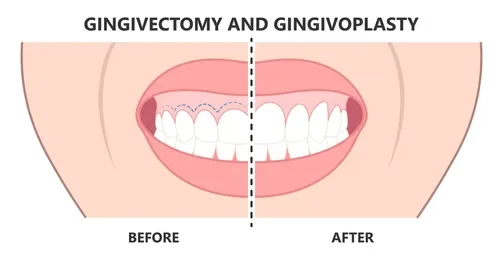
Gingivoplasty is a periodontal soft tissue surgery designed to reshape gum contours and restore natural gingival architecture when changes in gum appearance or function occur due to conditions such as gingival hyperplasia, periodontal disease, trauma, or developmental irregularities, and it is often used to improve the symmetry, health, and accessibility of gum tissue surrounding the teeth. Patients may seek evaluation for symptoms including excessive or uneven gum tissue, persistent inflammation, difficulty maintaining oral hygiene, or aesthetic concerns such as a “gummy smile,” and these symptoms may be caused by medication-related gingival enlargement, plaque accumulation, hormonal influences, genetic predisposition, or previous periodontal breakdown that altered the natural contour of the gums. A dental professional begins diagnosis with a comprehensive oral hygiene assessment, measurement of probing depths, evaluation for gingival inflammation, and consideration of underlying periodontal disease, often supported by diagnostic imaging to assess bone levels and determine whether the issue is isolated to soft tissue or linked to deeper structural changes. Gingivoplasty differs from gingivectomy in that gingivectomy focuses on removing diseased or excessive gum tissue, whereas gingivoplasty reshapes the tissue to create a more natural and functional contour after removal or reduction, though the two procedures may be performed together when clinically appropriate. Before gingivoplasty is performed, the dentist or periodontist ensures that active periodontal infection or uncontrolled inflammation is managed, as performing soft tissue surgery in the presence of untreated disease may increase the risk of postoperative complications. The procedure is typically done under local anesthesia, and depending on the case, the clinician may use a scalpel technique, laser gingivoplasty, or electrosurgery to precisely contour the gum margins, remove irregularities, and sculpt the tissue to follow the natural curvature of the teeth. Laser gingivoplasty has become increasingly common due to its ability to reduce bleeding, improve visualization, and potentially shorten healing time, while traditional scalpel methods remain effective and medically appropriate when performed by trained clinicians. Throughout the procedure, attention is given to maintaining healthy biologic width, protecting underlying bone, and ensuring gentle handling of tissues to support predictable healing. After the gum contour is reshaped, the surgical site may feel sensitive or slightly swollen, and postoperative symptoms can include mild discomfort, gum tenderness, or transient bleeding, all of which typically resolve with proper care. Patients are advised to follow postoperative instructions such as avoiding aggressive brushing near the surgical area, using antimicrobial mouth rinses if recommended, and maintaining soft food intake during the initial healing phase to minimize irritation. Most individuals experience noticeable healing within one to two weeks, though full maturation of the tissue may take longer depending on the extent of reshaping and individual healing factors. Risks associated with gingivoplasty include infection, delayed healing, gum recession if excessive tissue is removed, altered sensation, or temporary changes in gum color, though these risks are reduced through appropriate diagnosis, conservative tissue management, and adherence to postoperative care. Patients with underlying medical conditions such as diabetes, compromised immunity, or those taking medications that affect healing may require additional precautions or more frequent follow-up appointments. Gingivoplasty may also be recommended as part of a larger periodontal treatment plan, particularly when periodontal disease has caused irregular soft tissue contours that trap plaque and contribute to ongoing inflammation, making reshaping necessary to restore effective oral hygiene access. The procedure can support long-term oral health by reducing plaque retention points, creating smoother gum margins, and allowing patients to clean more effectively, which may contribute to better periodontal stability when combined with regular dental checkups and professional cleanings. In some cases, gingivoplasty is also used in conjunction with restorative treatments such as crowns or veneers, where proper gum contours are essential for achieving a functional and aesthetic outcome. Patients considering gingivoplasty often ask about its longevity, and while the results are typically stable, the long-term outcome depends on factors such as ongoing oral hygiene, control of any underlying conditions that contributed to gum enlargement, avoidance of tobacco, and adherence to regular periodontal maintenance. Understanding the purpose of gingivoplasty, the diagnostic steps involved, the procedural techniques used, the potential risks, and the expectations for healing helps patients engage in informed discussions with their dental provider and determine whether the procedure is appropriate for their specific concerns. Because gingivoplasty is a medical procedure requiring individualized planning, patients should consult with a qualified dental professional who can evaluate their oral health, review potential treatment options, and provide guidance that aligns with evidence-based standards and their long-term periodontal well-being, ensuring decisions are made responsibly and with full understanding of the clinical context.