Author:
Dr. Medvop Medical Team
Published Date:
25 Mar, 2026
Dental Implant
This article explains the medical indications, diagnostic steps, surgical procedure, risks, healing expectations, and long-term considerations associated with dental implants to support informed patient decision-making under the guidance of qualified dental professionals.
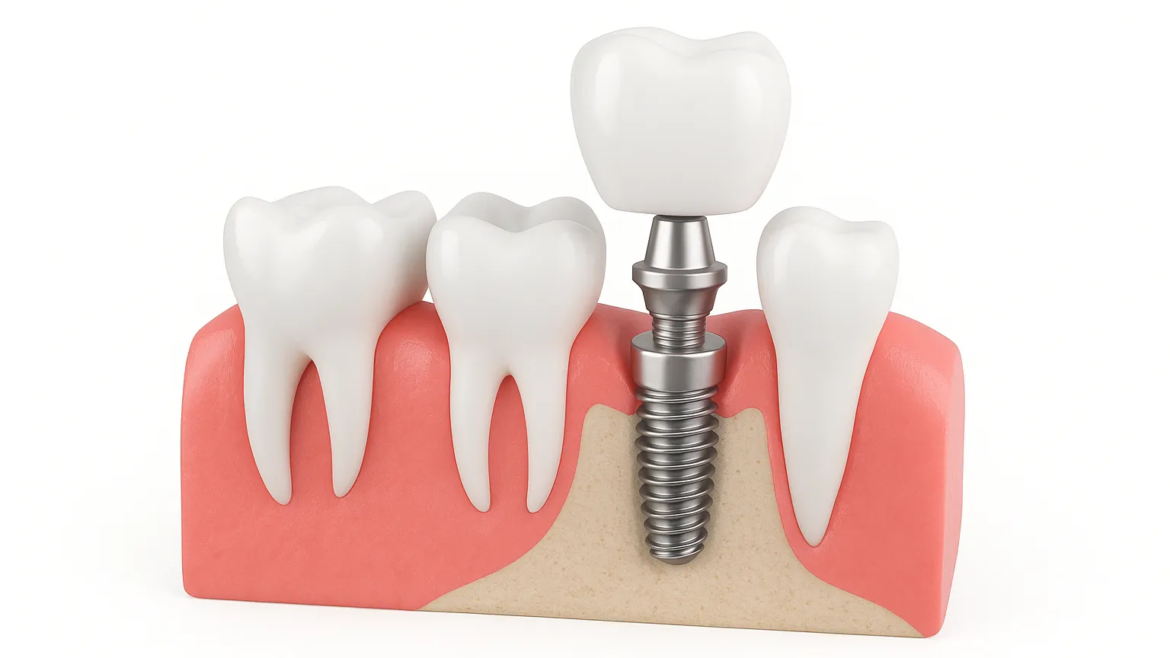
A dental implant is a medically supervised tooth replacement procedure used to restore function and aesthetics following tooth loss by placing a titanium implant into the jawbone, where it undergoes osseointegration, a biological process in which bone tissue gradually bonds to the implant surface. Dental implants may be recommended when tooth loss results from periodontal disease, trauma, extensive decay, failed root canal treatment, or congenital absence, and the goal is to replace a missing tooth with a stable foundation that can support an implant-supported crown or other prosthetic restoration. Before the procedure, a dental professional conducts a detailed assessment that typically includes a clinical examination, evaluation of gum health, analysis of jawbone density, and imaging such as periapical X-rays or cone-beam CT scans to identify anatomical structures, assess bone volume, and detect conditions such as bone resorption that may require bone grafting or sinus lift procedures. Symptoms related to tooth loss, including impaired chewing, shifting of adjacent teeth, bite changes, and difficulty maintaining oral hygiene, often motivate patients to seek implant treatment, but candidacy depends on factors such as systemic health, smoking habits, gum disease status, and the ability to maintain long-term oral hygiene. The dental implant procedure is usually performed under local anesthesia, during which the oral surgeon or implant dentist creates a precise opening in the jawbone and places the titanium implant, ensuring stable primary fixation without excessive pressure that could compromise bone healing. In cases where bone volume is insufficient, procedures such as bone grafting or sinus augmentation may be completed either before or during implant placement to improve long-term stability. After implantation, the healing period varies depending on bone quality, implant location, and individual biological factors; osseointegration typically requires several weeks to several months, during which postoperative symptoms such as mild swelling, discomfort, or temporary gum irritation may occur. These symptoms are generally manageable with routine postoperative care, and patients receive instructions that may include avoiding excessive chewing on the treated side, maintaining soft tissue cleanliness, and attending follow-up evaluations to monitor healing and detect early signs of complications such as infection, gum recession, or peri-implantitis, an inflammatory condition of the tissues surrounding the implant. Once adequate osseointegration has been confirmed, an abutment is attached to serve as the connection between the implant and the final prosthetic crown, bridge, or denture. The prosthodontic phase involves taking impressions or digital scans to create a restoration that aligns properly with the patient’s bite and distributes occlusal forces evenly to protect both natural teeth and the implant. Patients may have questions about the risks of dental implants, which can include infection, nerve injury, failure of osseointegration, sinus complications for upper implants, and mechanical issues such as screw loosening or fracture; however, careful diagnosis, appropriate case selection, and adherence to postoperative care significantly reduce the likelihood of complications. Conditions such as uncontrolled diabetes, active periodontal disease, tobacco use, or inadequate oral hygiene can increase risk, making comprehensive medical screening and ongoing maintenance essential. Dental implants also have long-term considerations, as implants can support function for many years when properly cared for, but their success depends on regular dental visits, evaluation of gum and bone health, professional cleanings, and management of contributing factors such as bruxism, which can place excessive stress on the implant and prosthesis. Alternatives to dental implants include fixed bridges, removable dentures, or doing nothing, each with its own advantages and limitations; implants may be preferred when preserving adjacent teeth and maintaining jawbone volume are clinical priorities. Patients often ask whether implants are better than dentures, and while implants can provide superior stability and chewing efficiency, the appropriate choice varies based on anatomy, financial considerations, and medical suitability. Throughout the process, evidence-based treatment planning ensures that each stage—from diagnosis and surgical placement to prosthetic restoration and long-term monitoring—supports oral health and functional outcomes. Patients considering a dental implant should understand the entire sequence, including diagnostic imaging, surgical placement, healing expectations, potential complications, and the need for lifelong oral hygiene and professional follow-up. Because dental implants are a complex medical procedure that requires individualized evaluation, patients should consult a qualified dental professional who can assess their specific needs, discuss treatment options, review risks and benefits, and plan care that aligns with their overall oral and systemic health, ensuring decisions are made responsibly and based on accurate clinical information.